WRITTEN BY: Harrie Phillips
BAdVocEd (VocEd&Trng), RVN, DipVN (Surgical, ECC), DipBus, DipTDD, TAA.

All veterinary nurses know that warming a patient during anaesthesia is important, but do you know when you should start actively warming your patients? Maintaining our patient’s body temperatures during anaesthesia is important – especially as there are multiple factors at play that can contribute to hypothermia.
Due to their large body surface to volume ratio, almost all our small animal patients will develop hypothermia under anaesthesia, unless we take steps to assist them in maintaining a normal temperature. In fact, one study of 1525 dogs showed that 83.6% presented with hypothermia post operatively. That rate was even higher for their feline counterparts – another study found that 96.7% of cats suffered hypothermia whilst under anaesthetic1.
Hypothermia can have devastating effects for our patients. It can affect the cardiovascular system, depressing heart conductivity, which lowers heart rate and cardiac output that in turn leads to a decrease in arterial blood pressure. Patients that are cold are also at a greater risk of developing cardiac arrhythmias, prolonged blood clotting times, and hypoventilation.
Hypothermia is an abnormally low body temperature. The normal range for rectal body temperature in cats is 38.1–39.2°C and for dogs is 37.9–39.9°C.
For a list of more reference ranges for a wide variety of species, refer to the Merck Veterinary Manual.
Hypothermic patients will take significantly longer to recover than a normothermic patient.
Hypothermia occurs because our patient’s ability to regulate their own body temperature is disrupted due to the effects of the anaesthetic drugs we administer to them. In addition to this, they will also lose heat due to direct contact with cold surfaces (such as the surgery and x-ray tables and cold cages); through exposure to cooler air around them and convection (warm air rises and cooler air replaces it); and evaporation through respiration and surgical incisions. Even how we perform our skin prep has a negative effect on a patient’s body temperature – wet fur and alcohol can hasten hypothermia.
A range of physiological changes occur under anaesthesia that also promote a drop in body temperature. The anaesthetic drugs we choose, such as acepromazine, can negatively impact thermoregulation and others such as opioids can depress metabolic heat production. Longer anaesthetics also contribute to higher rates of hypothermia (amongst other complications such as hypoglyceamia, hypotension and hypoxaemia). Vasodilation also results in excessive heat loss, and even muscle inactivity contributes.
Ok, so we get it, hypothermia is bad. So what can we do about it as veterinary nurses?
- Commence your temperature monitoring and steps to assist with maintaining body temperature at premedication. It has been shown that body temperature starts to drop after the premedicant has been administered. Keep your premeded animals in a draft free area, with plenty of warm bedding, and monitor their temperature.
- Monitor temperature throughout the anaesthetic and recovery period. Placing an oesophageal temperature probe is the easiest and best practice for continual temperature monitoring under GA. Monitoring should occur at least every 15 minutes and be recorded for trend identification. Otherwise regularly monitor rectal temperature along with the other vitals. Problems with rectal temperature monitoring for GA usually revolve around access – depending on what the surgical procedure is and the sterile field size. Luckily oesophageal temperature units are relatively cheap, or if you have a multi-parameter monitor, it’s likely you already have the capability.
- If a patient’s temperature is starting to decrease, start active warming immediately. Of course, prevention is better than cure, but if you detect a lower body temperature at any stage from premedication to recovery, you must instigate active warming.
- Minimise contact with cold surfaces.
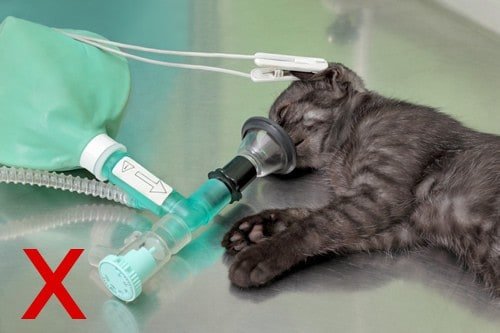 Don’t place your patients directly on cold surgical or prep tables or floors. The use of rubber mats, towels, and other layers to provide insulation from the cold is necessary. The veterinary team often forgets that the x-ray table is a cold surface too. Use towels and blankets between exposures and provide active warming if necessary. You can also purchase radiolucent x-ray mattresses which can not only increase patient comfort but provides an insulation layer.
Don’t place your patients directly on cold surgical or prep tables or floors. The use of rubber mats, towels, and other layers to provide insulation from the cold is necessary. The veterinary team often forgets that the x-ray table is a cold surface too. Use towels and blankets between exposures and provide active warming if necessary. You can also purchase radiolucent x-ray mattresses which can not only increase patient comfort but provides an insulation layer.
- Allow patients to urinate prior (or express the bladder). Urinating under anaesthetic or in recovery can contribute to wet fur and heat loss.
- Warm preoperative and intraoperative fluids. There are commercial units available that will warm fluids for intravenous administration. Vet nurses are also an ingenious mob, so there are plenty of ways you can warm your IV fluid lines. Just remember it must be safe for your patient and done close to the IV port. If running the line through a bowl of warm water – then remember to replace the water regularly as it cools.
- For intraoperative lavage fluids, ensure these are warmed to body temperature before use (around 38.5°C). If safe for the patient, these should be left in for several minutes before being suctioned out (warming your patient from the inside out is very effective).
- Microwaves should not be used to warm fluids, as they can superheat sections or overheat the fluids past 38.5°C – which is damaging to tissues. It is safer to have an incubator or warming cabinet, or use warm water baths to heat the fluids (monitoring the water temperature).
- Provide active warming during the anaesthetic.
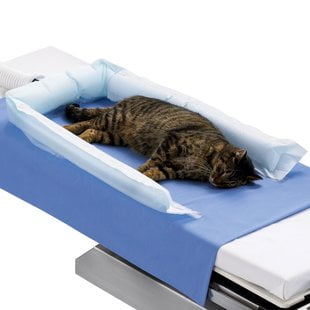 Active warming devices such as Bair Huggers® are the gold standard. These circulate warm air around your patient but make sure you maintain them properly and change filters at least yearly (all that fur can clog them and burn out the motor, or your clinic). You should also use a new blanket for each patient for infection control. Alternatives include devices like the HotDog® Warming blankets which are reusable electroconductive blankets that have even heat distribution and are flexible enough to facilitate positioning almost any way. They must be completely cleaned and disinfected between patients for infection control.
Active warming devices such as Bair Huggers® are the gold standard. These circulate warm air around your patient but make sure you maintain them properly and change filters at least yearly (all that fur can clog them and burn out the motor, or your clinic). You should also use a new blanket for each patient for infection control. Alternatives include devices like the HotDog® Warming blankets which are reusable electroconductive blankets that have even heat distribution and are flexible enough to facilitate positioning almost any way. They must be completely cleaned and disinfected between patients for infection control.
- If you are using a heat pad, ensure it is one designed for surgical and anaesthetic use and has an inbuilt thermostat to avoid overheating. Heated surgical tables are also available and should be on your wishlist. The use of hot water bottles, microwavable heat pads and bags should be discouraged as they are frequently overheated and can burn the patient. Anaesthetised and recovering patients are unable to move themselves away excessive heat, further increasing the risk of burns.
- Provide passive warming. The use of dedicated towels for the surgical suite to help cover the patient (under the drapes of course) can also help reduce heat loss. Cover as soon as you can and as much as you can without restricting access for monitoring or compromising the surgical site. You can also wrap limbs in bubble wrap or small blankets to help reduce peripheral heat loss. If your surgeon likes a colder theatre, it is even more important to provide insulation for your patient (or sneak the theatre temperature up to 22-24°C when they are not looking).
- When positioning your patient, using vacuum supports are not only easier to get the perfect position, but they also provide insulation. Probably worth adding some of these to your wish list too.
- Don’t get overzealous with your skin prep. Of course, you still need to perform an adequate skin preparation – but all at wet skin and fur will increase heat loss, as does the evaporative effect of alcohol. Try to not fling too much excess solution around, wetting fur unnecessarily. Where you can, use warm water to make up your scrubs and try to not leave too long between scrubbing and surgery. Dry off any unnecessarily wet fur before transporting to theatre.
- Match your anaesthetic equipment to your patient. Using a Universal-F or Bain style circuit can assist with warming inhalant gases before they reach th
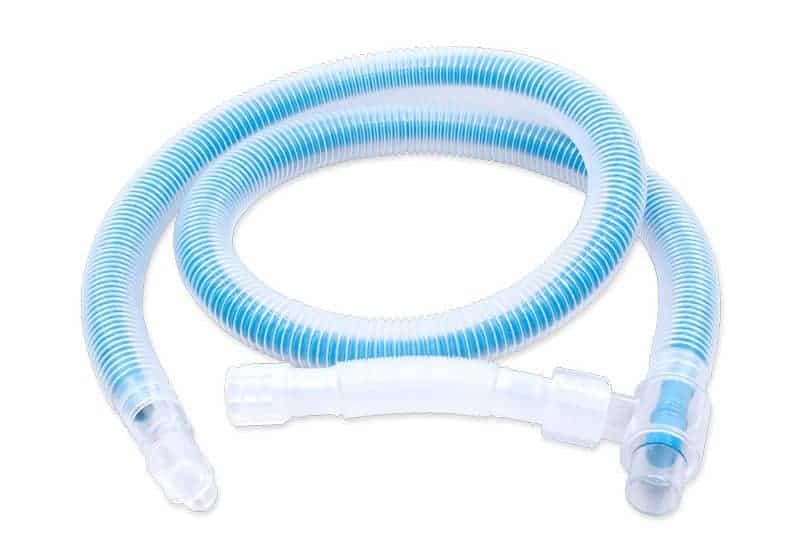 e patient, compared to traditional Y-circuits. Calculate your fresh gas flow rates (30mL/kg for rebreathing and 200mL/kg for non-rebreathing. Higher flow rates are not only wasteful, but are colder.
e patient, compared to traditional Y-circuits. Calculate your fresh gas flow rates (30mL/kg for rebreathing and 200mL/kg for non-rebreathing. Higher flow rates are not only wasteful, but are colder.
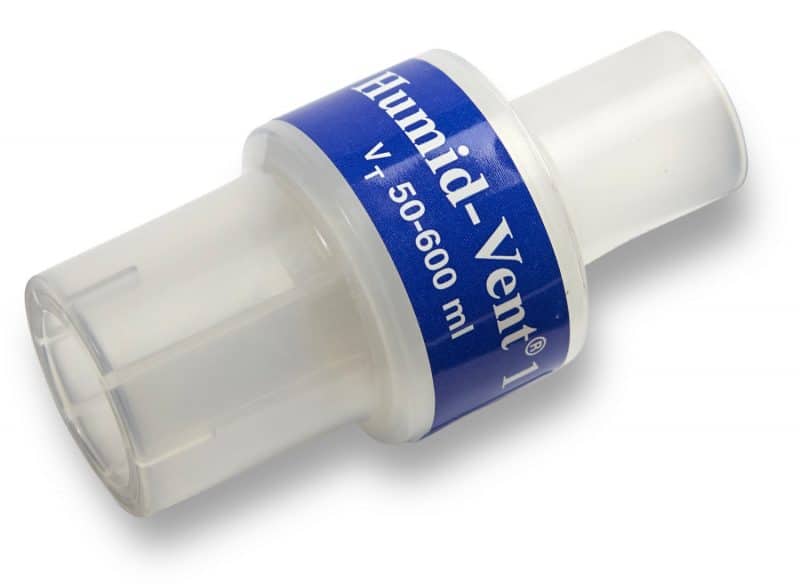 There are also funky devices called heat-moisture exchanges (HMEs) that sit between the ET tube and the breathing circuit. They help maintain body temperature by reducing evaporation from the respiratory tract and increasing heat. They are single use only however, as they can harbor microorganisms, so don’t forget to charge them out to the owner.
There are also funky devices called heat-moisture exchanges (HMEs) that sit between the ET tube and the breathing circuit. They help maintain body temperature by reducing evaporation from the respiratory tract and increasing heat. They are single use only however, as they can harbor microorganisms, so don’t forget to charge them out to the owner.
- Be organized. We want to keep our anaesthetic time to a minimum. We can’t control the vet, but we can be organised and predict their needs – cutting down on any waiting around time.
- Don’t forget recovery! You need to monitor your patient’s temperature every 15-30 minutes until they are almost normothermic. Up until this point, you must provide warming. Monitoring is vital as we can easily overheat our patients in recovery and hyperthermia is also dangerous.
- Remove heating when your patient’s temperature is 1°C off normal (so around 37°C) to prevent over warming. You need to monitor for at least 30 minutes past removing all the heating to ensure the patient is maintaining their own temperature.
- Recovery should be in a warm, draft free area of the clinic and have plenty of blankets available. Dry off your patient as soon as you can, and get them covered up. It is a good idea to ensure the recovery bed is ready, waiting and warm before you arrive, so ask your fellow nurses or ward assistants to have it prepared, along with any warming devices.
- Food! Unless contraindicated, once the patient is fully conscious, with a gag reflex and able to hold up their own head, offer some food. The digestion process kick starts metabolism and can shorten recovery time and assist with heat production.
References
1. J. I. Redondo, P. Suesta, I. Serra, C. Soler, G. Soler, L. Gil, R. J. Gomez-Villamandos. Retrospective study of the prevalence of postanaesthetic hypothermia in dogs. Veterinary Record, 2012; 171 (15)
Header Image credit: HotDog Warming Blanket – image courtesy of http://www.wm-referrals.com
want to learn more?
ANAESTHESIA & SURGICAL ANALGESIA
SHORT COURSE
This course introduces students to the foundations of anaesthesia – how to set up and test the equipment, what circuits to pick and when, calculations, and other factors that can influence how stable our anaesthetics are. You’ll also learn how the drugs we use affect the body, patient warming techniques and important and why premedication is necessary. We also explore analgesia specific for surgical patients.
Check it out